by Active Alignment | May 11, 2020 | Exercises, Health, Therapy, Uncategorized
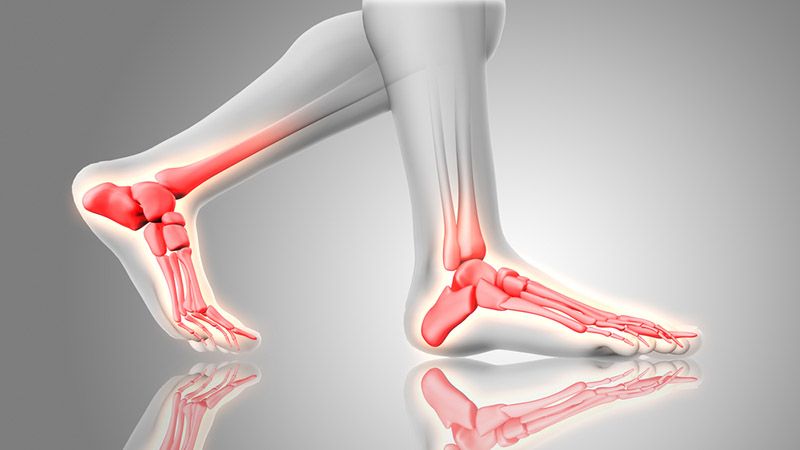
The medial longitudinal arch (inside arch) is the main shock absorbing structure in the foot. The ability of the arch to shock absorb is dependent on the amount of movement from the bones that make up the first ray. What is the first ray? The first ray is the segment...
by Active Alignment | May 5, 2020 | Exercises, Health, Therapy, Uncategorized
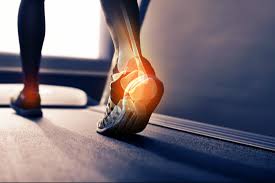
As Pedorthists, this condition represents a major portion of our daily schedule. We are here to tell you that your condition (although experienced by many) is unique, just like you and should be treated as such! When you experience heel pain what is the first thing...




